Melanoma treatment has changed dramatically over the past decade. Alongside groundbreaking immunotherapies such as checkpoint inhibitors, another fascinating approach has emerged — using a modified virus to attack cancer cells.
This treatment is called Talimogene laherparepvec, more commonly known as T-VEC or by its brand name Imlygic.
It may sound surprising, but in certain patients with melanoma, this therapy can help the immune system recognise and destroy cancer.
What Is T-VEC?
T-VEC is a type of oncolytic virus therapy, meaning it uses a virus that has been genetically modified to infect and destroy cancer cells.
Scientists created T-VEC from a weakened form of the herpes simplex virus type-1, the virus that normally causes cold sores. However, the virus has been altered so that it preferentially infects melanoma cells while leaving normal cells largely unharmed.
When injected into a melanoma tumour, the virus:
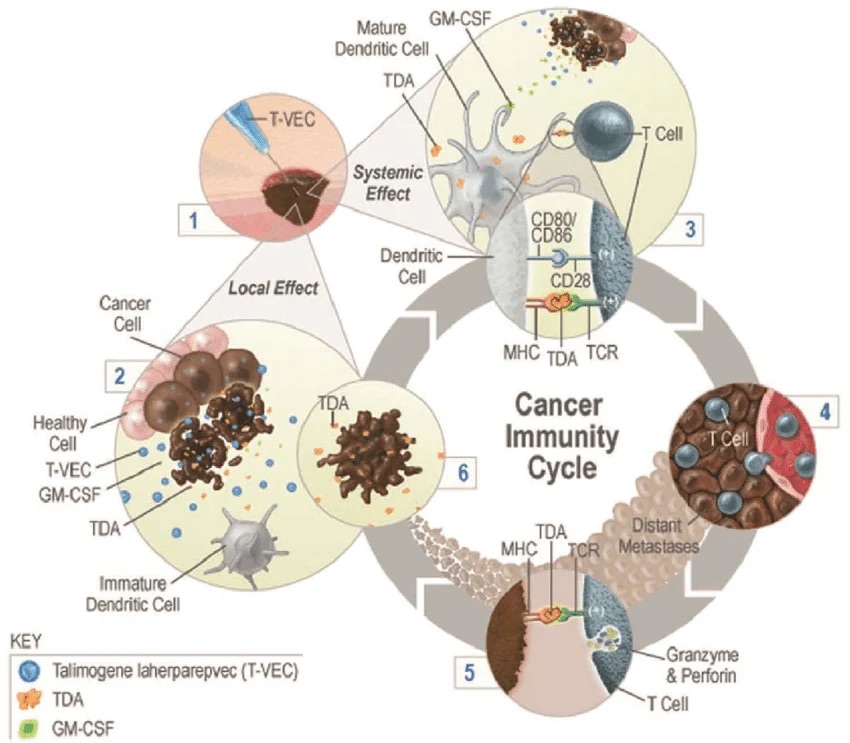
Enters the cancer cells Replicates inside them Causes the cancer cells to burst (lysis) and die.
As the tumour cells break apart, they release cancer antigens that alert the immune system and help it recognise melanoma elsewhere in the body.
How T-VEC Stimulates the Immune System

T-VEC does more than simply kill cancer cells.
The modified virus has been engineered to produce a protein called GM-CSF (granulocyte-macrophage colony-stimulating factor). This protein stimulates immune cells to attack melanoma.
This creates a two-step anti-cancer effect:
1️⃣ Direct tumour destruction
The virus infects melanoma cells and causes them to rupture.
2️⃣ Immune activation
The immune system learns to recognise melanoma cells and may begin attacking tumours elsewhere in the body.
This is why T-VEC is often described as both a local treatment and an immunotherapy.
Who Is T-VEC Used For?
T-VEC is typically used in people with unresectable melanoma, meaning tumours that cannot be removed surgically.
It is most suitable when melanoma appears as skin lesions, subcutaneous lumps, or lymph node tumours that can be injected directly.
It is worth pointing out that this treatment is not very effective when used against mucosal melanoma.
In the UK, the treatment is approved for adults with Stage IIIB Stage IIIC Stage IV M1a melanoma provided the cancer has not spread to major internal organs such as the brain, lungs, or liver.
How the Treatment Is Given?
Unlike most cancer therapies that are given through an IV drip, T-VEC is injected directly into melanoma tumours.
A typical treatment schedule looks like this:
First injection Second injection three weeks later Then injections every two weeks
Treatment usually continues for at least six months, or until there are no injectable tumours remaining or the treatment is no longer effective.
Doctors may inject several tumours during one session, depending on how many are present.
How Effective Is T-VEC?
Clinical trials have shown encouraging results for patients with injectable melanoma lesions.
In the major OPTiM clinical trial, T-VEC achieved:
- Higher durable response rates compared with GM-CSF injections.
- Reduction in the size of many injected tumours.
- Some shrinkage of nearby untreated lesions as well.
Research is also exploring combining T-VEC with checkpoint inhibitor immunotherapies such as Nivolumab, Pembrolizumab, and Ipilimumab, which may enhance overall immune responses.
Possible Side Effects
T-VEC is generally well tolerated compared with many cancer treatments.
The most common side effects include:
- Flu-like symptoms
- Fever and chills
- Fatigue
- Pain or redness at the injection site
Occasionally, more serious reactions such as skin infections around the injection site can occur.
Because the treatment contains a modified virus, patients are also advised to keep injection sites covered and follow hygiene precautions to prevent viral transmission.
A Unique Step Forward in Melanoma Treatment

T-VEC represents a fascinating example of how modern medicine is learning to turn biology against cancer.
By combining direct tumour destruction with immune system activation, this therapy offers another option for people whose melanoma cannot be removed surgically.
And as research continues, scientists hope that combining T-VEC with other immunotherapies will unlock even greater benefits for patients.
💙 Final Thought
Melanoma treatment has evolved rapidly, bringing hope to many patients who once had very limited options. T-VEC is just one example of the innovative therapies now being explored in the fight against this disease.
Every new treatment reminds us that science is steadily climbing the mountain toward better outcomes and longer lives for people living with melanoma.