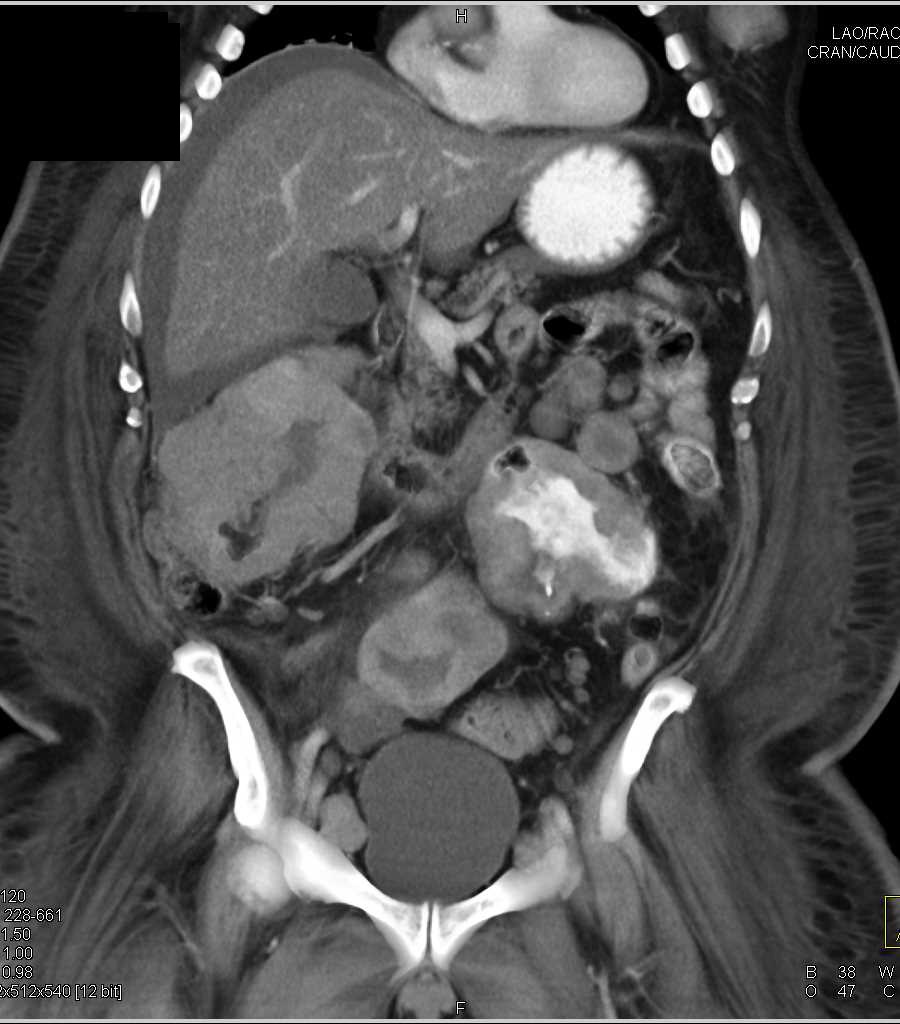
So, after my PET Scan which confirmed “volume uptake” of the radioactive mixture in various parts of my body including the masses in my bowel, neck lymph nodes and an area in my right leg by the femur came the request for the biopsy.
The PET CT Scan helps doctors diagnose and assess various conditions, particularly cancers, by identifying areas of abnormal function and providing detailed information about their location and severity but it does not confirm the actual type of cancer.
Confirming the exact nature of the cancer involves a biopsy which is then sent to histology for a closer examination which will help the team determine the exact nature of ongoing treatment.
The biopsy of melanoma involves several steps in the pathology process. Here’s how doctors and pathologists make the diagnosis:
1. Microscopic Examination (Histopathology)

A dermatopathologist examines the biopsy tissue under a microscope. They look for specific features of melanoma, such as:
- Abnormal melanocytes (pigment-producing cells)
- Asymmetry in the cells
- Irregular borders
- High mitotic rate (cells dividing quickly)
- Pagetoid spread (melanocytes moving upward in the skin layers)
This is the primary and most reliable method of confirming melanoma.
2. Special Stains (Immunohistochemistry)

If the diagnosis isn’t completely clear, the pathologist may use special stains that detect proteins typical of melanoma cells. Common melanoma markers include:
- S100 – a protein family used as a marker for diagnosing melanoma, with S100B also being a prognostic marker for advanced disease.
- HMB-45 – a melanoma-specific immunohistochemistry stain used to identify melanoma pathology, particularly by highlighting immature melanocytes in the epidermis and upper dermis.
- Melan-A (Mart 1) – The NHS uses a panel of stains, including Melan-A, to identify a tumor’s origin and confirm if it is cancerous, especially when distinguishing it from other conditions like benign moles or other skin cancers.
- SOX10 – can be more sensitive than S100 for certain metastatic melanomas.
These stains help distinguish melanoma from benign moles or other cancers.
3. Deeper Tissue Levels

Sometimes additional deeper sections of the biopsy are cut and reviewed to see the full architecture of the lesion.
4. Second Opinion (Dermatopathology Review)
If the result is uncertain or clinically important (e.g., stage 4 patient, recurrent disease), a second expert may be asked to review the biopsy. This is very common with melanoma.
5. Molecular or Genetic Testing (in some cases)

If the melanoma is confirmed, additional tests might be done to help guide treatment—like checking for:
- BRAF mutation – change in the BRAF gene found in about half of all melanoma cases that causes melanoma cells to grow uncontrollably.
- NRAS – NRAS mutation in melanoma occurs in about 15–20% of cases and is associated with more aggressive tumors.
- KIT – These mutations are more common in specific subtypes of melanoma, such as mucosal and acral melanomas, particularly in older individuals and those with a history of chronic sun damage (CSD).
These don’t confirm melanoma but help plan therapy.
In my case the results of the biopsy of the cancer involves my bowel have confirmed that my melanoma has now invaded my bowel and requires treatment other than surgical removal as there are more than one “deposit”.
Immunotherapy beckons …… IPINIVO here I come.
Please subscribe to my site to catch the next stages of my cancer experiences. It’s free and I just hope to educate and inspire others.